News
-
 April 5, 2024Apr 5, 2024
April 5, 2024Apr 5, 2024Ways to reduce health care disparities in minorities
Health care disparities are complex for many reasons, including lack of access, historical injustices and bias within the health care industry.
Read More -
 April 5, 2024Apr 5, 2024
April 5, 2024Apr 5, 2024Meet Generations on Line CEO & founder Tobey Dichter
Generations on Line is a nonprofit organization that reduces isolation by providing easy, fast and free digital skills for older adults.
Read More -
 April 5, 2024Apr 5, 2024
April 5, 2024Apr 5, 2024Satisfying alternatives to empty-calorie snacks
Guidelines and recipes to help you choose a healthier option to snack on.
Read More -
 April 5, 2024Apr 5, 2024
April 5, 2024Apr 5, 2024Making websites accessible for people living with disabilities
Guidance on web accessibility and the ADA to help businesses that are open to the public create websites that are accessible to people living with disabilities.
Read More -
 April 5, 2024Apr 5, 2024
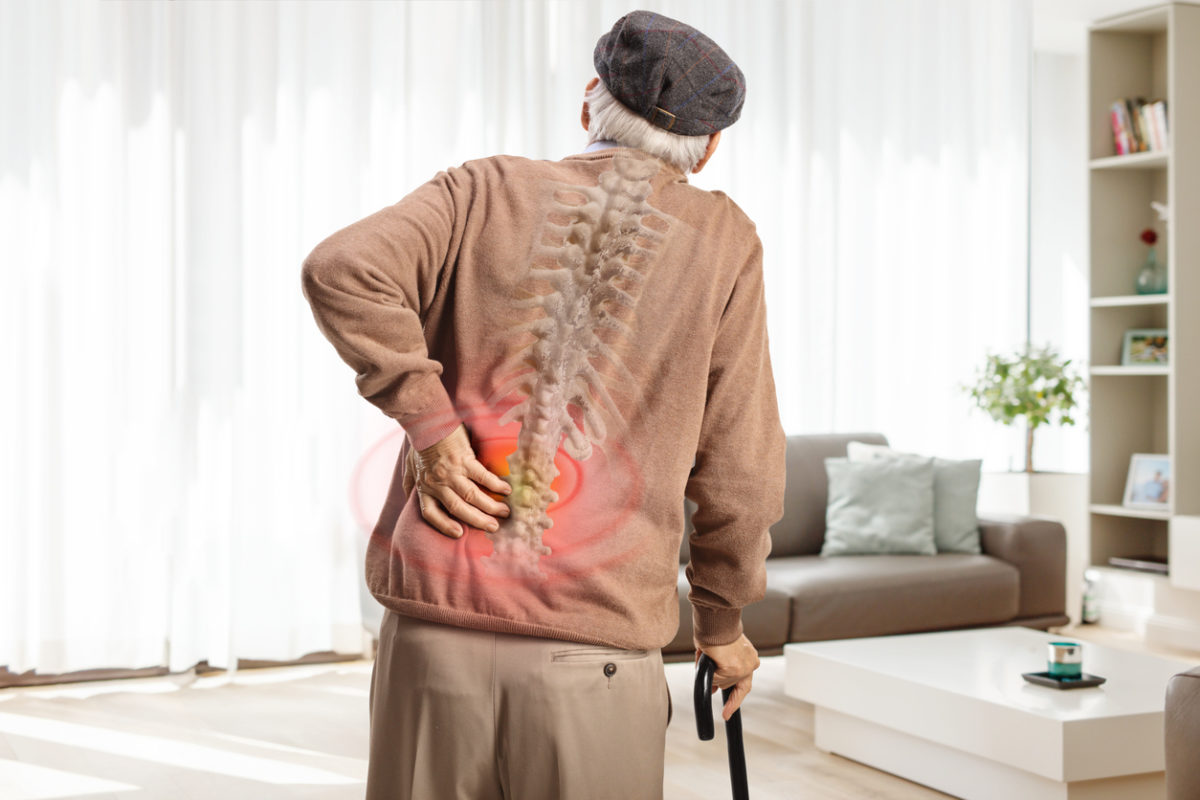
April 5, 2024Apr 5, 2024Got back pain? There are many approaches to treating it
Back pain can be a consequence of aging, being overweight, having either very physical job or a sedentary job, or weak abdominal and back muscles.
Read More -
 April 5, 2024Apr 5, 2024
April 5, 2024Apr 5, 2024How to spot the grandparent scam
Scammers can use voice-cloning software to make themselves sound like your loved one.
Read More -
 April 5, 2024Apr 5, 2024
April 5, 2024Apr 5, 2024Social Security in 2024: What you need to know
April is Social Security month, and this year brings some new Social Security changes. Here is a rundown of what you need to know for 2024.
Read More
